
Sperm from donor with cancer-causing gene was used to conceive almost 200 children
2025-12-10 05:06:53
James GallagherHealth and science reporter
 shutterstock
shutterstockA sperm donor who unwittingly carried a genetic mutation that significantly increases the risk of cancer has fathered at least 197 children across Europe, a major investigation has revealed.
Some of the children have already died, and only a minority of those who inherited the mutation will survive cancer in their lifetime.
The sperm was not sold to UK clinics, but the BBC can confirm that a “very small” number of British families who were informed used donor sperm during fertility treatment in Denmark.
The European Sperm Bank in Denmark, which sells sperm, said the affected families expressed their “deep sympathy” and acknowledged that sperm had been used to create too many children in some countries.
 Getty Images
Getty ImagesThe investigation was conducted by 14 public broadcasters, including the BBC, as part of the European Broadcasting Union’s Investigative Journalism Network.
The sperm came from an anonymous man who was paid to donate it while he was a student, starting in 2005. The women then used his sperm for about 17 years.
He is in good health and has passed donor screening tests. However, the DNA in some of his cells mutated before he was born.
It damaged the TP53 gene, which plays a crucial role in preventing the body’s cells from turning into cancerous cells.
Most of the donor’s body does not contain the dangerous form of TP53, but up to 20% of his sperm do.
However, any child formed with affected sperm will have the mutation in every cell in his or her body.
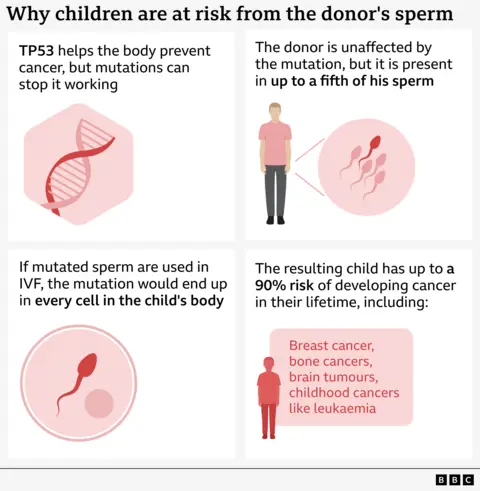
This condition is known as Li-Fraumeni syndrome, and it carries a 90% chance of developing cancer, especially during childhood as well as breast cancer later in life.
Professor Clare Turnbull, a cancer geneticist at the Institute of Cancer Research in London, told the BBC: “It’s a shocking diagnosis.” “It’s a very difficult diagnosis for the family, there’s a lifelong burden of living with this risk, and it’s obviously devastating.”
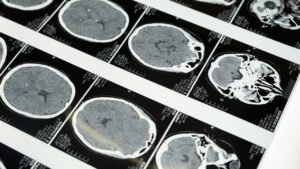
MRI scans of the body and brain are needed every year, as well as abdominal ultrasound, to try to detect tumors. Women often choose to have their breasts removed to reduce their risk of cancer.
The European Sperm Bank said that “the donor himself and his family members are not sick” and that such a mutation “is not preventively detected by genetic screening.” They said they “immediately suspended” the donor as soon as they discovered the problem with his sperm.
The children have died
Doctors who were seeing children with cancer linked to sperm donation raised concerns at the European Society of Human Genetics this year.
They reported that they had found 23 children infected with the variant out of 67 known at the time. Ten of them have already been diagnosed with cancer.
Through freedom of information requests and interviews with doctors and patients, we can uncover a much larger number of donor-born children.
This number is at least 197 children, but this may not be the final number because data was not obtained from all countries.
It is also unknown how many of these children have inherited this dangerous type.

Dr Edwige Kaspar, a cancer geneticist at Rouen University Hospital in France, who provided the initial data, told the investigation: “We have many children who have already developed cancer.
“We had some kids who actually had two different cancers and some of them actually died at a very young age.”
Céline, not her real name, is a single mother in France whose child was born with donor sperm 14 years ago and has the mutation.
She received a phone call from the fertility clinic she used in Belgium urging her to get her daughter tested.
She says she has “no hard feelings at all” toward the donor, but says it was unacceptable to receive sperm that “wasn’t clean, safe, or risky.”
She knows that cancer will haunt them for the rest of their lives.
“We don’t know when, we don’t know which one, and we don’t know how many,” she says.
“I understand that there is a high chance that this will happen, and when it happens, we will fight, and if there are multiple people, we will fight several times.”
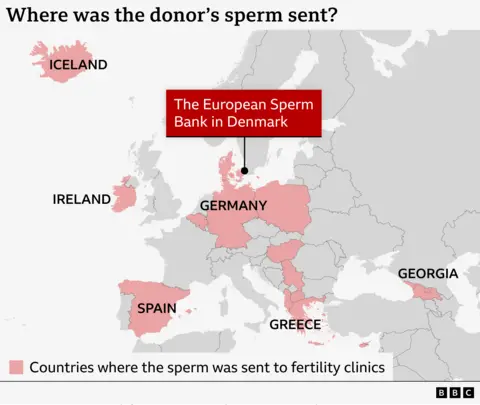
Donor sperm has been used in 67 fertility clinics in 14 countries.
The sperm was not sold to UK clinics.
However, as a result of this investigation, authorities in Denmark notified the UK Human Fertilization and Embryology Authority (HFEA) on Tuesday that British women had traveled to the country to receive fertility treatment using donor sperm.
These women have been informed.
Peter Thompson, chief executive of the HFEA, said a “very small number” of women were affected and “were told about the donor by the Danish clinic where they were treated”.
We do not know whether any British women have received treatment in other countries where donor sperm has been distributed.
Concerned parents are advised to contact the clinic they have used and the fertility authority in that country.
The BBC has chosen not to disclose the donor’s identification number because he donated in good faith and known cases in the UK have been contacted.
There is no law limiting the number of times donor sperm can be used worldwide. However, each individual country sets its own limits.
The European Sperm Bank acknowledged that these restrictions had been “unfortunately” violated in some countries and that it was “in dialogue with the authorities in Denmark and Belgium”.
In Belgium, one sperm donor is supposed to be used by only six families. Instead, 38 different women gave birth to 53 children for the donor.
The UK limit is 10 families per donor.
“You can’t check everything”
Professor Alan Pacey, who ran the Sheffield Sperm Bank and is now vice-chancellor of the University of Manchester’s School of Biomedicine and Health, said countries had become reliant on large international sperm banks, and half of the UK’s sperm was now imported.
He told the BBC: “We have to import sperm from large international banks, who also sell it to other countries, because that’s how they make their money, and that’s where the problem starts, because there’s no international law about how many times you can use sperm.”
He said the case was “terrible” for everyone involved, but it would be impossible to make sperm completely safe.
“You can’t screen for everything, we only accept 1% or 2% of all men who come forward to donate sperm in the current screening arrangement, so if we made it more stringent, we wouldn’t have any sperm donors – that’s where the balance lies.”
This case, along with that of a man who was ordered to stop after fathering 550 children through sperm donation, has once again raised questions about whether there should be stricter limits.
The European Society of Human Reproduction and Embryology recently proposed a maximum of 50 families per donor.
But she said this would not reduce the risk of inheriting rare genetic diseases.
It would even be better for the well-being of the children who discover they are one of hundreds of half-siblings.
Sarah Norcross, director of the Educational Progress Fund, an independent charity for people with infertility and genetic conditions, said: “More needs to be done to reduce the number of families with same donor births globally.”
She told the BBC: “We don’t fully understand what the social and psychological implications of having these hundreds of half-siblings are. It is potentially traumatic.”
The European Sperm Bank said: “It is important, especially in light of this issue, to remember that thousands of women and couples do not have the opportunity to have a child without the help of donated sperm.
“It is generally safe to have a child with the help of donor sperm if the sperm donors are screened according to medical guidelines.”
What if you are considering using a sperm donor?
Sarah Norcross said these cases are “extremely rare” when you consider the number of children born to a sperm donor.
All the experts we spoke to said that using a licensed clinic means your sperm will be screened for more diseases than most future fathers.
Professor Pacey said he would ask, “Is this a British donor or is it a donor from somewhere else?”
“If it’s a donor from somewhere else, I think it’s legitimate to ask questions about has this donor been used before? Or how often will this donor be used?”
If you or someone you know is affected by the issues, help and support details are available at BBC action line.
https://ichef.bbci.co.uk/news/1024/branded_news/906d/live/ff8d66c0-d4ed-11f0-8c06-f5d460985095.jpg
























إرسال التعليق